ICSI Intracytoplasmic sperm injection
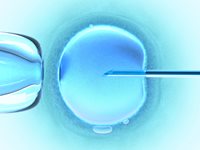 What is ICSI?
What is ICSI?
ICSI is a procedure that is used with in vitro fertilisation (IVF) in which one sperm is injected directly into one egg in order to fertilise it. The technique has been especially useful for men with very low sperm counts and low motility, since ICSI ensures that the sperm reaches the egg directly rather than waiting for the sperm to naturally fertilise the egg. Thus, ICSI is sometimes used as a treatment method for male infertility. ICSI is now used as part of nearly half of all IVF treatments.
Which infertility problems can ICSI help?
ICSI can help overcome many problems causing male infertility such as:
- low sperm count
- low sperm motility
- No sperm in semen
- damaged or absent vas deferens
- retrograde ejaculation
- irreversible vasectomy
- immunological factors (e.g. anti-sperm antibodies)
- other conditions that prevent the fertilisation of the egg
How is ICSI done?
As with normal IVF, the woman is given fertility drugs to stimulate her ovaries to produce several mature eggs for fertilisation. The man would then produce a semen sample by masturbating into a sample pot. If the man does not have sperm within his semen, then it may be possible for the doctor to retrieve sperm from his testicle under an anaesthetic.
The woman is then given an anaesthetic to remove the eggs using a fine hollow needle. Ultrasound is used to help the doctor locate the eggs. Within the laboratory a scientist then injects one single sperm into the egg (ICSI); this is done several times to produce up to 10 possible embryos. The sperm and egg are then placed into an incubated within a Petri dish and checked the following day to look for signs of fertilisation. If fertilisation has occurred then an embryo (group of cells) will have formed, which can be seen under a microscope.
The procedure is then the same as IVF, embryos which have formed can be transplanted into the woman’s uterus through the cervix using a thin catheter.
A maximum of three embryos can be placed back into the uterus, however many clinics are now moving towards only putting one or two embryos back. Multiple births carry a greater risk to both the mother and the babies. Any embryos which are left can be frozen and used in future treatments, in case the cycle is not successful.
ICSI success rate
ICSI has the highest fertilisation rate of 60-70%; however pregnancy success rates are similar to that of normal IVF. This is because there are other factors which effect success such as the fertilised embryos developing properly and the embryo implanting in the uterus correctly. Therefore the success rate of ICSI is similar to IVF in the region of 25%, depending upon age.
Benefits of ICSI
ICSI enables couples to achieve parenthood who would not otherwise do so due to male factor infertility. Men with very low sperm count are able to have their own genetic child by using ICSI.
It is also possible to retrieve immature sperm from the testes, enabling men to have a child who have previously had a vasectomy.
ICSI has also helped couples have a child who have experienced unexplained infertility.
Risks of ICSI
ICSI involves taking one sperm and inserting it directly into the egg. Under normal fertilisation sperm have to compete and only the strongest and healthiest sperm makes it through the cell wall into the egg. It is thought that there may be a higher risk of congenital and health problems for the resulting child due to this procedure.
A research study showed that 4.2% of children born from ICSI had a malformation which mainly affected boy’s urinary and genital systems. This was a 3 fold increase compared to children conceived naturally. The same study found that ICSI babies had more childhood illnesses and needed more medical intervention before the age of 5.
The long term effects of ICSI have yet to be properly seen or researched.
For many parents the advantages of having their own genetic child far outweigh the risks of ICSI.